For many – perhaps most – suffering is the biggest worry about life’s end. Suffering doesn’t start and end with pain management. It includes peace of mind and comfort – both of which are highly individual, and can hold the keys to perception of and requirements for a ‘good death’:
- What comforts you, or what brings you comfort?
- What are your small pleasures, or what gives you pleasure?
- What brings you peace of mind?
Comfort and feeling good about herself is the gift a palliative doctor gave to a terminally ill patient who wanted no further medical treatment. He simply asked:
“What would make this a good day for you?”
“If I could sing”
The patient, Dolly Baker (nee Thelma Botelho), was once a renowned songstress. And sing she did.
I have sat in countless meetings, workshops, think tanks, round-tables where everything but the word, comfort is used to help us on the way to as good a death as possible. Amongst the questions commonly asked:
What are your values?
What are your beliefs?
What’s important to you?
What are your goals of care?
These may may all play into what makes us feel good, and brings comfort, but these approaches often then require further probing and questioning which takes so much more of that precious thing that’s often in short supply: health care professionals time.
Revealing answers, reveal simple solutions
Answers about comfort reveal solutions that:
often have nothing to do with medical interventions;
can bring comfort and joy to attending healthcare professionals;
can help family and friends support more purposefully and meaningfully;
As a ‘layperson’ whose focus is end-of-life education, I regularly suggest changing the direction of end of life conversations from ‘what’s acceptable to you medically’ to ‘what brings you joy and comfort.’
West Park Health Center chose the Theory of Comfort for interviews with self-selected patients in their complex continuing care facility. The results, summarized in a poster presentation at a conference on improving care for the frail elderly , were both revealing and individual. While harder to identify trends and collect meaningful data, the approach laid the groundwork for more of the same, based on the impact on quality of life.
These interview questions were a comfort-related series, with nurses asking one or two questions per ‘visit’ – taking no more per-patient time than allotted.
Patients were initially puzzled by the simplicity of the question. Were they missing something? Was it a trick? But when reassured that the intent was as straightforward at it seemed, the responses were immediate and – for the most part – do-able, although sometimes in a more reduced form.
“Mrs B. always liked a fuss made about her birthday. Her family’s scattered so she can’t have the big party she’d like, but we’re working with Recreation Therapy to arrange Skype and FaceTime birthday wishes and we’re getting a helium balloon and a card signed by all healthcare professionals.”
A patient who could only eat pureed food, longed to see a veal chop, spaghetti and mashed potatoes on her plate. The staff sourced machines that create food shapes from puree. ‘Feeling the rain’ is another request that was easily fulfilled.
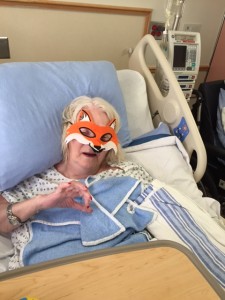
I sit on West Park’s Palliative and Supportive Steering Committee and fellow member – Psychologist Dr Sharon Jankey – shared the story of how her mother’s Halloween mask helped distract from the discomfort of an IV PICC line and had a double effect: it cheered the hospital staff, too.
 Life is made up of more what’s ‘wrong’ with us. Comfort can be the route to finding out what makes us feel ‘right’.
Life is made up of more what’s ‘wrong’ with us. Comfort can be the route to finding out what makes us feel ‘right’.
Here’s Dolly Baker, who died a more peaceful death – a ‘good’ death – within a month of her song.
