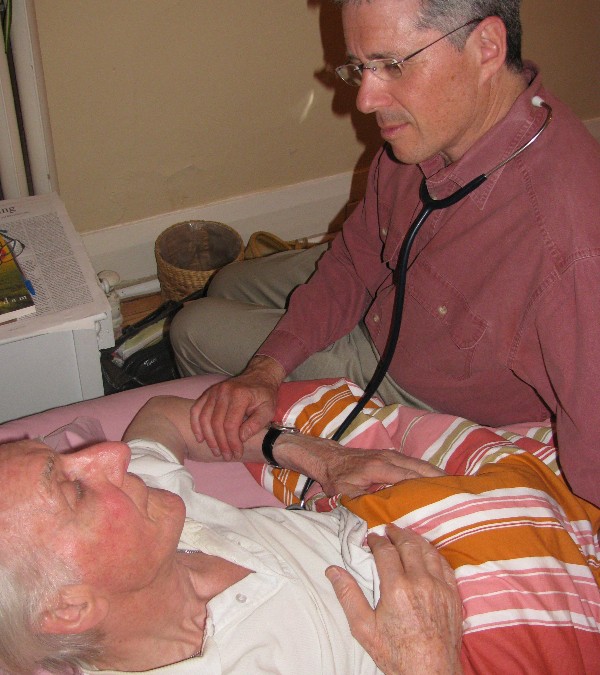
“What I fear the most – what really terrifies me – is being short of breath and not being able to swallow.”
So said the husband of his dying wife. This is terrifying to me, too, so I listened closely to the response given by Palliative Care physician, Dr Sandy Buchman:
“I can help with shortness of breath: there are medications that change the perception of that feeling of breathlessness. It doesn’t change the underlying cause, but I see patients whose breathing is still labored yet they say they’re now feeling fine. About swallowing: eventually, your wife will not be able to eat. That’s normal, and I can help both of you cope with that. “
I am in the privileged position of being invited to ‘ride’ with Dr Sandy Buchman on palliative house calls. Working at a teaching hospital, he often brings residents as part of their learning experience, but I am the only layperson to get this access. And what an experience it was: learning more about the palliative approach – to symptom management and to that all-important aspect of any meaningful interaction: communication.
We decided my best introduction would be ‘educator’ and, although a bit apprehensive about intruding at a fraught time, I was universally welcomed. In a couple of the visits, I was able to employ ‘active listening’ with family members feeling comfortable enough with me to share insights that proved helpful.
A range of palliative patient and family situations
- A B, 100 years old, on oxygen, was a renown pathologist;
- L.M., 88, bed-bound, the right side of his face paralyzed, was key economist to a head of state.
- C.D. 89, on oxygen and bedbound, patriarch of 5 successful children, sings in answer to questions.
- V, 67, ecstatic about a procedure to ease the pain of her hollowed out bones, is ‘mistress’ of a vast estate north of the city;
- DR 47 with back pain from cancer, worries that dogs aren’t getting any walks. The mother of 5 – two of whom are in prison, the other three live in her subsidized apartment
Buchman, a family physician who embraces palliative care, is a committed team member,
“I’m ‘just’ the doctor- she’s the Boss.”
He refers to fellow healthcare professional who coordinates all aspects of care and equipment, according to the patient and family needs.
Sandy brings to each home visit an unhurried atmos a bottle of hand sanitizer and a knapsack with his computer.
Dressed in jeans and a shirt, he looks more a college student that a physician who’s been president of both the provincial and federal Colleges of Family Physicians.
“Coming in to someone’s home instead of in my office shifts the power”
At one house, we’re greeted by another member of the palliative team who is clearly anxious.
“Before you go in, I just want to warn you they’re very angry” Says Sandy, “Take a deep breath and try to be where they’re ‘coming from’. Don’t take it personally.”
What happens over the next hour will happen again and again at each house. And each time, I see tensions rise and fall and flare and then cool down as Dr Buchman shepherds patient and family through education about palliative care, where ‘doing nothing is not an option’ ensuring they understand its scope and focus: comfort and to support living the best right to the end. He then hones in on specific needs of the patient and family, walking them through scenarios while making it clear, again
“The patient is The Big Boss.”
Checking medications: asking to see all medications, not just relying on a list
Carefully explaining his thoughts and reasons for modifying medication doses, while trying to ensure those assembled understand:
“Everything is an experiment: we start low and go slow.”
In one instance, the patient dismisses a medication that should help her pain control. When her daughter explains it in such a way that it resonates with the patient, Dr Buchman gives full props to the daughter: just one example of the empowering communication strategy that comes second nature. He also reassures the patient:
“I will respect your decision. Don’t ever worry about that.”
I see the patient relax: she doesn’t have to worry about disappointing the doctor or having to lie to him.
With being immobile, as are most, and with most taking constipating pain medication, Buchman makes sure there’s a strategy to help poop – which often requires several approaches.
Before doing a quick mini physical that includes checking the mouth, he asks about mouth care – often overlooked and often needing relief from dry or sore mouth.
“Is there anything I’ve left out? Any symptoms or any discomfort I should know about?”
Answers go beyond the medical and being able to share is a big relief:
“It’s driving me crazy not to be active: I was always on the go.”
Sometimes there’s a solution:
“I love to read but I can’t hold a book anymore.” A tablet (iPad) provides the answer.
“My mother was always the center of things.” The solution: Consider putting her bed in the dining room so she can be in the center of activity.”
During the visit, Buchman uses different communication approaches to acknowledge the reality of life’s end being at hand.
- “You have a life-limiting condition”
- “You know this is what you’ll pass away from”
- “ This is a terminal condition.. I see that you understand that.”
- “You’re not going to get better”
The scenarios he describes helps patient and families wrap their heads around the ‘what if’s, and usually starts with:
“It’s 3am: While the palliative team is on call 24/7 there are situations that require a decision of whether or not to go the hospital.”
For many, going into – or back into – the hospital is the worst possible scenario. Tho not always:
“I don’t want my children to see me ‘like that’” prompts a note to apply for Hospice
The most common reasons for hospitalization are:
- Breathlessness
- Fever
- Pain
- Infections – respiratory or bladder
- Falling and breaking a hip
In more than one of the visits, he’s asked to check on something other than what’s on his list: feet that seem unduly cold;
- angry red discolouration on legs
- a swelling on the back of the head
- a sensitive heel, made sore by contact with the bedsheets
Blood pressure is taken at every visit, with a common comment:
“My pressure’s always better when you take it.” Sandy grins and explains: “I try to just work it into a comfortable, relaxed conversation, so you practically don’t know it’s happening. Taking it when you’ve just gotten to the examining room in the doc’s office is the worst time.”
At another visit, where two church members are visiting and reading the patient psalms, one of the ladies takes note of how thorough Dr Buchman is:
”He doesn’t just ask for a list of medications: No! He wants to see them all. That’s much better.”
“You have such a comforting presence” says another – the wife of a dying man.
Dying doesn’t mean giving up on life: rather, each of these palliative visits Buchman makes every effort to determine what the patient and family enjoyed, what are their worries. Those who are still able to speak clearly appreciate this interest and concern: shoulders relax from up around ears. There’s often laughter.
“We can get some medical marijuana – that can help with sleep.” Explains Buchman. “If there’s any left, we can give it do dad” guffaws the daughter.
Another visit, we’re greeting at the building door by the patient herself. “This is unusual.” With a diagnosis of lung cancer, she wants to be given the straight goods: Buchman caveats with:
“We are very bad at prognosis – estimating death – but in general terms 6 months.”
With this answer she relaxes and says;
“This is the first time I feel I’ve been listened to – that you’re interested in me – my worries. I’m a stubborn woman and this is helping me to get over my reluctance to accept help.”
Thorough. Reassuring. Listening. Observing. Addressing. Solving. Never dismissing.
Dr Buchman smiles:
“I tell my medical students: This is just good patient care”